HAND HYGIENE PROTOCOLS
It is no secret that Long-Term Care residents represent a high-risk population when it comes to COVID-19 and other public health threats. Further, residents are at an increased risk in terms of severe infection, hospitalization, and death. It is important to be proactive in order to protect them and an effective hand hygiene program must be a key component of the protection plan.
Hand hygiene protocols are intended to reduce the transmission of microorganisms and associated infections which can lead to increased morbidity, mortality, lengths of hospital stays, and overall costs. The protocols should consist of specific recommendations that are based on scientific evidence and expert consensus.
The Hand Hygiene protocols listed below address the core elements of hand hygiene and behaviors. Indications for handwashing and hand antisepsis are:

The Importance of Hand Washing
Healthcare facility employees constantly work with their hands. They are likely to become prime carriers of bacteria and other unwanted microorganisms. For example, nursing staff touch up to 15 different surfaces during a single patient/ resident interaction. This means the average nurse will touch 912 different surfaces during a routine 12-hour shift. Unwanted germs, including the virus that causes COVID-19 can be directly spread from a nurse’s hands to equipment and other surfaces in a resident room or to the resident themselves.
Since person-to-person contact is the most significant risk factor in infection control, correct hand washing plays a major role in reducing infection incidence rates.
Hand Washing Technique
A splash of water will not do the job. Rather, effective hand washing requires a comprehensive process.
The correct hand washing process begins with wettings one’s hands. Soap is then thoroughly applied to all areas of the hand. The soap may be dispensed as a liquid, or the healthcare facilities may use new soap tissues. Bar soap should not be used since it can quickly become contaminated. If necessary, use a brush to clean difficult areas such as under the nails.
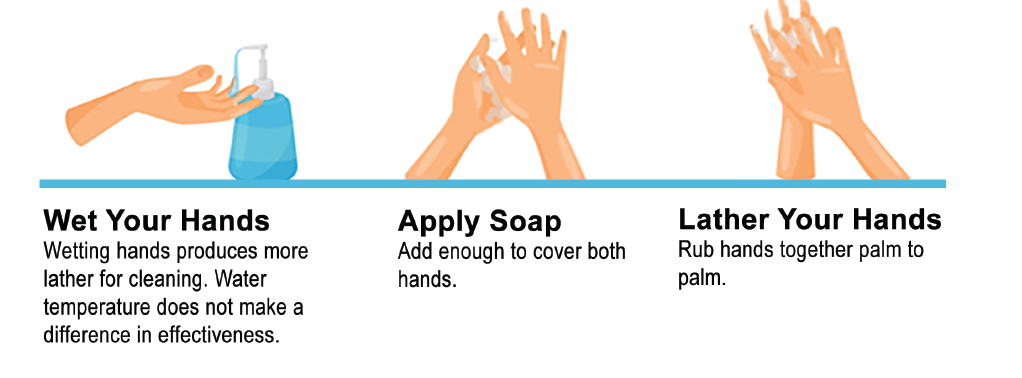
With a rotating motion, rub the hands together while counting to twenty. Apply adequate friction to this rubbing. Extend the wash area to a minimum of two to three inches above the wrist. Interlace the fingers and rub up and down to ensure the hands will be clean between the fingers.
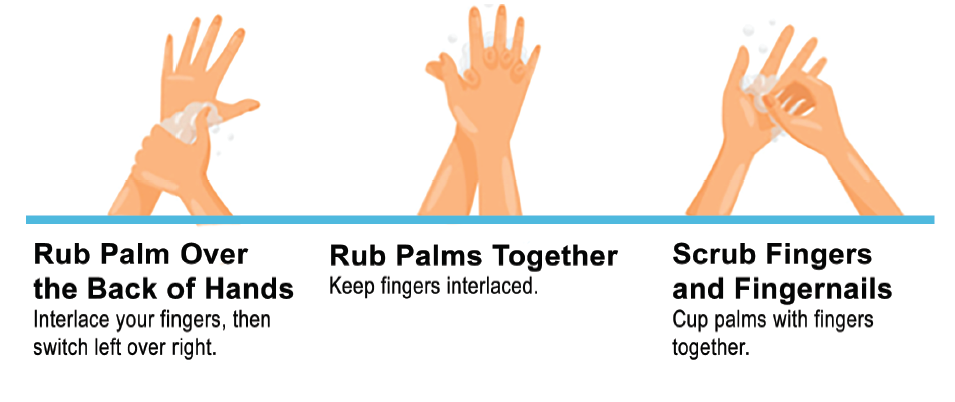
After scrubbing is complete, rinse the hands well and dry them thoroughly with a clean paper towel. Do not turn off the water with clean hands as that would undo the work just completed. Turn the faucets off using a clean paper towel.
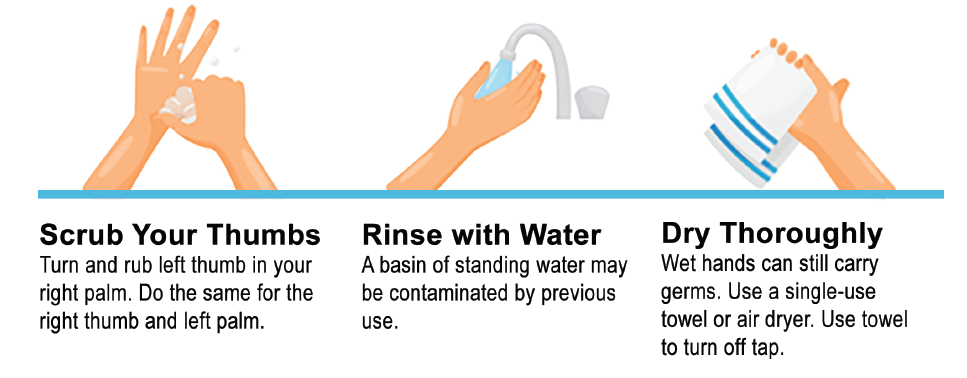
When leaving the room, open the door using another clean towel. Prop the door open with a foot as the towel is discarded and leave without touching the door. Remember, if the hands become re-contaminated, the individual will need to begin the hand washing cycle again.
Hand washing must be done before and after performing each duty. Wearing rubber gloves can reduce the frequency of hand washing but will not eliminate it altogether. To break the chain of infection, and to protect the hands, correct hand washing techniques cannot be over-stressed.
Alcohol-Based Hand Sanitizers
Alcohol-based hand sanitizers (ABHS) are effective against the virus that causes COVID-19, as well as other germs. They can provide immediate killing effect and are less dependent on technique.
Healthcare facilities should consider making hand sanitizer dispensers available inside and outside of resident rooms – at an easily accessible location. Alcohol-based hand sanitizers can also require less drying and can be less damaging to skin.
Germs, however, can escape the cleaning effects of ABHS and handwashing when sheltered under long fingernails. Individuals should, therefore, avoid wearing artificial nails when caring for residents.
Gloves
- Gloves protect our hands but DO NOT replace hand hygiene
- DO clean your hands with every glove change
- DO NOT wear the same pair of gloves for more than one patient/ resident
- DO NOT touch yourself while wearing gloves
- DO NOT use soap and water to re-use gloves
Assessing Thoroughness and Other Aspects of Hand Hygiene
Following effective hand hygiene practices has long been recognized as the most important way to reduce the transmission of pathogens in health care settings.
It is as important to assess the technique with which health care workers perform hand hygiene as it is to measure when and how often they perform it. One way to assess and teach proper technique is to observe the staff periodically.
Healthcare Workers Hand Hygiene practices can be improved through efforts such as continual education, providing timely feedback, constant reminders, and structured approaches to performance improvement
The Partners in Protection Hand Hygiene Protocols are intended to address the core elements of hand hygiene behaviors.




